Salt gets a bad rap, but sodium is an utterly essential mineral in the body. The electrolyte is crucial for maintaining fluid balance, carrying nerve impulses, and supporting proper muscle contractions.
 |
|
|
But while the body needs enough of the mineral to carry out these functions, getting too much sodium in your diet can damage your health.
Below, experts break down four signs you’re eating too much salt — and what to do about it.
Tip
FYI: Salt and sodium aren’t the same thing. Table salt is made of sodium chloride, not sodium alone. A teaspoon of salt contains about 2.3 grams of sodium, per the Cleveland Clinic. We’ll use the two terms interchangeably here, but know they aren’t one in the same.
1. You’re Thirsty All the Time
It’s not exactly breaking news that eating salty foods makes us feel parched. But why exactly does this happen?
Well, when the concentration of the blood starts to rise (thanks to an increase in solutes like sodium, for example), the brain and kidneys start working to restore balance.
Antidiuretic hormone, for example, may be activated so the body retains fluids that help dilute the spike in sodium. Neural signals can also fire to promote sensations of thirst, according to a December 2016 study in Current Biology.
To prevent dehydration, you may start to feel physical symptoms such as dry mouth and dry skin, Tracy Lockwood Beckerman, RD, registered dietitian and author of The Better Period Food Solution, tells LIVESTRONG.com. That’s your body telling you to drink up in order to rehydrate your cells.
2. You Feel Bloated
Ever noticed that your rings fit extra snug after a salty meal?
“The more sodium you consume, the more water you will carry,” Kate Patton, RD, a registered dietitian with the Cleveland Clinic’s Center for Human Nutrition, tells LIVESTRONG.com. That’s because water follows salt due to osmosis (sixth grade biology, anyone?).
While it may seem counterintuitive to drink more water when you feel bloated, it can actually counteract the effects of eating too much salt. Consuming adequate fluids can flush everything — including excess sodium — out of the system.
“To help combat feeling bloated, drink a lot of water, go for a walk after that meal or drink some tea with lemon,” Beckerman recommends.
3. Homemade Food Tastes Bland
The salt shaker isn’t the main culprit when it comes to Americans’ high sodium intake. Rather, it’s the sodium found in processed and packaged foods (think: canned soups, frozen meals, snack foods and deli meats) that makes up the majority of our sodium consumption.
In fact, people who ate greater amounts of ultra-processed foods were found to have a significantly higher likelihood of having high blood pressure, per a large December 2016 study published in the American Journal of Hypertension. (More on that connection below.)
“Whole foods like fruits, vegetables, whole grains, and raw nuts and seeds are naturally low in sodium,” Patton says.
That’s great, but it can pose problems for those who are accustomed to eating processed and restaurant foods.
“The exposure of fried, saucy or overly salted foods can cause your taste buds to get used to a certain level of salt,” Beckerman notes. The result? Home-cooked meals taste bland — likely causing you to resort to takeout yet again. Cue the vicious cycle.
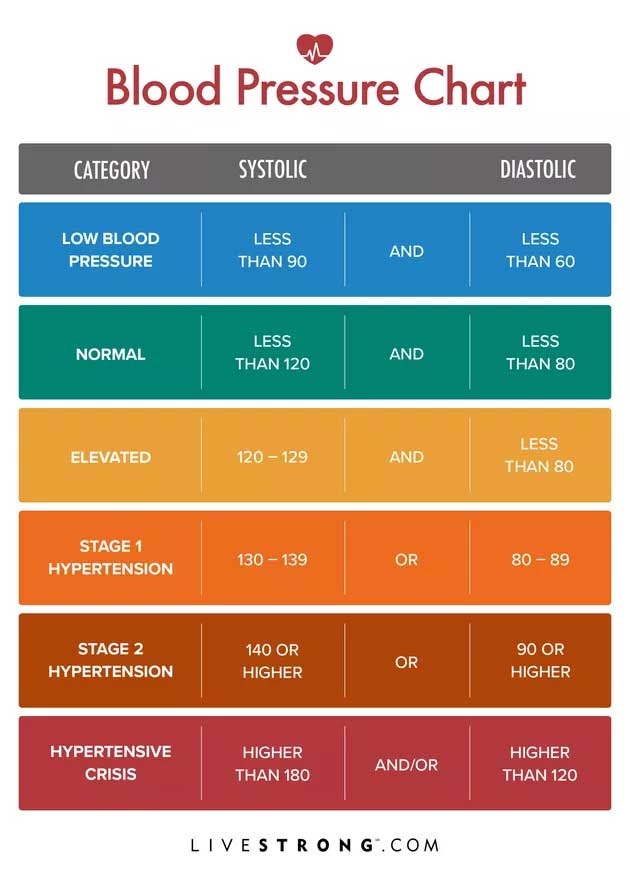
4. Your Blood Pressure Is Rising
Salt isn’t the only thing that can influence blood pressure — genetics, stress, weight, alcohol intake and physical activity levels also factor in, per Harvard Health Publishing. But chronic consumption of high-sodium foods can play a big role.
“Excess sodium intake promotes volume retention, which is a major factor in high blood pressure, or hypertension,” Luke Laffin, MD, a preventative cardiologist at the Cleveland Clinic, tells LIVESTRONG.com.
All that extra fluid can exert force on the blood vessels. Over time, this pressure can obstruct the normal flow of blood and oxygen to organs, making it even harder for the heart to pump and the kidneys to restore fluid and electrolyte balance, according to the Cleveland Clinic.
“Long-term uncontrolled hypertension predisposes individuals to increased risk of strokes, heart attacks, heart failure and chronic kidney disease,” Dr. Laffin says. “Although the association is not as clear, certain data suggest uncontrolled hypertension can increase one’s risk of dementia or cognitive impairment.”
Tip
Healthy blood pressure is lower than 120/80 mm Hg. The first number, called systolic BP, represents the amount of pressure during a heart contraction. The second number, called diastolic BP, represents the amount of pressure when the heart relaxes between beats.
 |
|
|
So, How Much Salt Is Too Much Salt?
The American Heart Association (AHA) recommends Americans consume less than 2,300 milligrams of sodium daily. That’s about the amount in just one (!) teaspoon of table salt.
Even that number may be high, though.
An “ideal” salt intake clocks in at about 1,500 milligrams of sodium per day, especially for those who have high blood pressure, according to the AHA. For reference, a mere 1-cup serving of canned soup can serve up some 650 milligrams of sodium, nearly half of your recommended intake for the entire day.
How to Reduce Your Sodium Intake
1. Look for Sneaky Sources of Salt
You’re likely well aware that potato chips tend to be rich in sodium, but there are plenty of less obvious sources out there too. Patton says to beware of the below if you’re trying to dial back your sodium intake:
- Breads, rolls, wraps, bagels
- Canned or jarred tomato sauces
- Breakfast cereals
- Cottage cheese
- Ketchup
- Prepared salad dressings
2. Check Nutrition Labels
It’s helpful to determine what your baseline sodium intake is and then start finding alternatives or substitutions to lower your intake as necessary, Patton says. Also, begin tuning in to the information provided on nutrition labels.
“A food is considered ‘low sodium’ if it has less than 140 milligrams of sodium per serving,” Patton notes.
Tip
While lifestyle and dietary changes are crucial for managing blood pressure levels, it’s also important to work with a doctor or registered dietitian who can provide professional guidance, especially if you have hypertension.
3. Swap Salt for Spices
While the salt shaker isn’t the enemy, it’s not a bad idea to reduce your usage if you tend to salt your food a ton while cooking at home.
“Sub out salt by warming up to spices and herbs such as basil, rosemary, paprika, and turmeric and use those in your meals,” Beckerman suggests. “Adding in aromatics such as garlic, onions, shallots, and leeks will add a ton of flavor without the salt.”
4. Cook Differently
Finally, if you’re looking to mimic restaurant-style eats at home without overdoing the salt and added fats, consider investing in an air fryer, slow cooker, or dehydrator.
“These methods of cooking don’t require the use of excessive salt or oil in order to yield a delicious meal,” Beckerman says. “That way you can prepare your food without compromising your health and the taste.”
References:
- American Heart Association: “Shaking the Salt Habit to Lower High Blood Pressure”
- Harvard Health Publishing: “Salt and Your Health, Part 1: The Sodium Connection”
- American Journal of Hypertension: “Ultra-Processed Food Consumption and the Incidence of Hypertension in a Mediterranean Cohort: The Seguimiento Universidad de Navarra Project”
- Current Biology: “Thirst”
- American Heart Association: “Hypertension Guideline Resources”
Important Notice: This article was originally published at www.livestrong.com by Anthea Levi, RD where all credits are due.