Mental stress and anger may have clinical implications for patients with heart failure, according to a new report. Read on to know more.
A new study at Yale University says that mental stress and anger may have clinical implications for patients with heart failure. Heart failure is a life-threatening cardiovascular disease in which the heart is damaged or weakened. This can lead to a reduced ejection fraction, in which the heart muscle pumps out a lower amount of blood than is typical with each contraction. In this study of patients who had heart failure with reduced ejection fraction, researchers evaluated the effects of stress and anger on diastolic function.
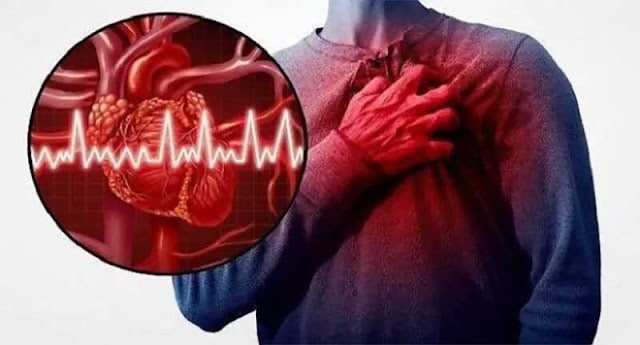 |
| Diastolic heart function describes the ability of the heart to relax and refill between muscle contractions and is predictive of mortality risk. @Shutterstock |
Diastolic heart function describes the ability of the heart to relax and refill between muscle contractions and is predictive of mortality risk. The Journal of Cardiac Failure published this study.
Stress Affects Diastolic Function
For one week, participants completed daily questionnaires about their experiences of stress, anger, and negative emotions during the previous 24 hours. They completed a standardized “mental stress” protocol in which they solved challenging arithmetic problems and described a recent stressful experience. Echocardiograms were performed to assess diastolic function at rest and during the stress task.
Patients who reported experiencing anger in the week prior to the laboratory mental stress protocol exhibited worse baseline resting diastolic blood pressure, the researchers said. Furthermore, most patients demonstrated stress-provoked changes in diastolic function, including decreased early relaxation and increased diastolic pressure.
Mental Stress Is Common In Patients Of Heart Failure
According to researchers, mental stress is common in patients with heart failure due in part to the complexities of disease self-management, progressively worsening functional limitations, and frequent symptom exacerbations and hospitalizations. There is evidence that patients who experience chronically elevated levels of stress experience a more burdensome disease course with diminished quality of life and increased risk for adverse events.
Clarifying the relevant behavioral and physiological pathways is especially important in the era of COVID-19 when the typical stressors of heart failure may be further compounded by pandemic-related stressors.
Stress Management Important To Improve Clinical Outcome
Factors such as mental stress and anger often go unrecognized and are under-addressed. This study contributes to the extensive literature showing that stress and anger affect clinical outcomes for patients with heart disease, adding chronic heart failure to the list that includes ischemic heart disease (narrowed arteries) and arrhythmic disease.
While stress management and related techniques have been shown to reduce the risk for adverse events among patients with ischemic heart disease (narrowed arteries), further work is needed to identify factors that increase vulnerability to the effects of stress in heart failure, and to determine whether stress management can improve outcomes for these patients.
A Few Stress Management Tips
You need to manage your stress if you want to keep your heart healthy and avoid the risk of heart failure. Exercise regularly and eat a healthy diet. Don’t let your work pile up. This is often a common reason for stress. Try out some relaxation techniques like yoga and meditation. Listen to soothing music and take a walk in the midst of nature. All these steps will help you live a stress-free life.
Important Notice: This article was originally published at www.thehealthsite.com by Jahnavi Sarma where all credits are due.