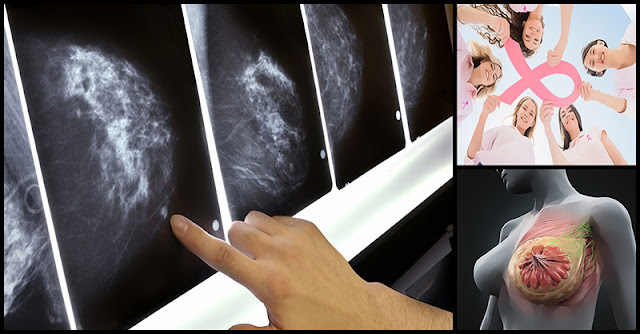
One of the longest and largest studies conducted in the field of mammography that involves 90,000 women in 25 years finally concluded that mammograms have no impact on breast cancer mortality. The study revealed that the death rate from breast cancer is the same between those who did not receive an annual mammogram and to those who did while 22 percent that is screen-detected breast cancers were over-diagnosed that eventually leads to unnecessary treatments. The researchers also concluded that “the data suggest that the value of mammography screening should be reassessed.”
There is also a big question about whether mammography screening really benefits women. According to a Cochrane Collaboration review, it was found out that there is no evidence that mammography screening affects the overall mortality on breast cancer patients.
In the U.S., the American Cancer Society recommends annual mammograms for women considered as average-risk starting at the age of 40. On the other hand, the US Preventive Services Task Force recommends mammogram screening for women at the age of 50 at an interval of every other year.
These recommendations confuse women whether mammogram screening can really be of help or in contrary, be harmful. This is the reason why the Swiss Medical Board made a straightforward recommendation: no more systematic mammography.
Why Did the Swiss Medical Board Do Away with Routine Mammograms?
The Swiss Medical Board noted that they became “increasingly concerned” about what they are finding after a year of reviewing all available evidence and its implications about the mammogram. The said “evidence” isn’t sufficient to back up the global consensus of other experts in the field that suggests mammogram is safe and is actually capable of saving lives.
Based on the data they gathered, mammography appeared to prevent only one death for every 1,000 women that have gone through screening while causing harm to many more. This comprehensive review led them to recommend that no new systematic mammography should be introduced and existing programs should follow a proper time limit.
Sadly, many women are still uninformed that the science that supports the health benefits of mammograms is utterly lacking. Instead of being told of what the truth is, women are misled and guilt-tripped into thinking that it is a medical irresponsibility when they skip their annual mammogram. This tactic is really hard to go against, especially when you are overly concerned about your personal health.
However, when it comes to cancer prevention, doctors are just as confused and manipulated as the average person on the street because of the overwhelming industry and media propaganda that ignores or outright downplays any research that intensely contradicts their profit-based agenda.
Five Important Facts About Mammograms That Every Woman Should Know
Before your next (or first) mammogram, you may be interested to know the following:
1. Mammograms May Not Work if You Have Dense Breasts
Mammogram screening is hard to decipher if the patient has dense breast tissues and 50 percent of women have it. Cancer cells and dense breast tissue both appear white on an X-ray, making it nearly impossible for a radiologist to detect cancer in these women. It’s like trying to find a snowflake in a blizzard.
Breast density laws have been passed in California, Connecticut, New York, Virginia, and Texas, making it mandatory for radiologists to inform their patients who have dense breast tissue that mammograms are basically useless for them. A law is now being considered at a federal level as well.
2. Mammograms May Offer Less Benefit Than You Think:
According to a survey done on women, most of them said that they believe mammography reduces the risk of breast cancer death by at least half and prevents death per 1,000 women screened. The truth is, mammography may, at best, offer a relative risk reduction of 20 percent and only prevent in absolute terms only one breast-cancer death per 10,000 women.
3. False Positives are Common (and Dangerous)
In the U.S., where advancement in medical technology is at its peak, the risk of having a false-positive test in 10 mammogram screening is still a concerning 58 to 77 percent! When a woman is told that she may have breast cancer based on the result of the screening, this means that there is almost more than half probability that it is a false-positive. They will then be subjected to more testing such as biopsy or surgery, which unnecessarily carry their own set of risks.
4. Mammography May Increase the Risk of Breast Cancer in Women with a BRCA 1/2 Mutation:
The British Medical Journal published results showing that women carrying a particular gene mutation called BRCA ½ – which is linked to breast cancer – are more vulnerable to radiation-induced cancer.
Women carrying this specific mutation were twice likely to develop breast cancer when exposed to diagnostic radiation (this includes mammograms) before the age of 30 as compared to those who did not have this gene. They further stressed out that the radiation-induced cancer was relative to the amount of exposure and dosage, meaning the greater the dose and exposure, the higher the risk of developing breast cancer.
5. There are Other Screening Options
You have the right to utilize other screening options. Always remember that only a biopsy can confirm cancer. Screening tools only aid in the process of showing concern.
Your Waist Size Is Linked To Your Breast Cancer Risk
Breast cancer is the most prevalent cancer in women, and obese women are 60 percent more likely to develop this type of cancer as compared to those who have a normal weight. Getting a mammogram is not the same as prevention. In order for you to really avoid breast cancer, you need to really focus on a real prevention measure and not just early detection. One way of doing this is by maintaining a healthy weight, particularly a healthy waist size.
It is reported in TIME magazine:
“An increase in skirt size was the single most predictive measure of breast cancer risk, the study concluded. When women went up a single skirt size over a 10-year span between their mid-20s and mid-60s, they were shown to have a 33% greater risk of developing breast cancer after menopause. Buying two skirt sizes up during that same period was linked to a 77% increased risk.”
The Sugar Connection
Obesity is driving up the rates of breast cancer in many developed countries. And what is the root cause of obesity? There are many factors that contribute to obesity but there is one that particularly plays a major role in it – SUGAR. According to researchers, adults who drank at least one sugar-sweetened beverage per day are 27 percent most likely to become obese or overweight.
If health agencies really want to make a considerable impact on breast cancer, they need to focus on sharing the truth about sugar (including grains) and their role in cancer and obesity. Unfortunately, breast cancer is a multi-billion business, and mammography is one of its main profit carriers. This is the reason why the industry is fighting over just to keep it, even if it means downplaying or ignoring the truth.
Avoiding Sugar and Other Top Breast Cancer Prevention Tips
Most cancers, including breast cancer, can be prevented by strictly applying basic common sense and healthy lifestyle strategies. No available screening method, whether mammography or otherwise, is going to lower your risk of developing cancer but the tips below will definitely do.
- Avoid sugar, especially fructose, and processed foods.
- Optimize your vitamin D levels.
- Limit your protein.
- Avoid unfermented soy products.
- Improve your insulin and leptin receptor sensitivity.
- Exercise regularly.
- Maintain a healthy body weight.
- Drink a pint to a quart of organic green vegetable juice daily.
- Get plenty of high-quality, animal-based omega-3 fats, such as krill oil.
- Pack up on Curcumin.
- Avoid drinking alcohol.
- Avoid synthetic hormone replacement therapy, especially if you have risk factors for breast cancer.
- Avoid BPA, phthalates, and other xenoestrogens.
- Make sure you’re not iodine deficient.
- Avoid charring your meats.